Robert Koch, Creation, and the Specificity of Germs
Abstract
Microbiology is dominated by evolution today. Just look at any text, journal article, or the topics presented at professional scientific meetings. Darwin is dominant.
Keywords: microbiology, evolution, Robert Koch, Koch’s postulates, anthrax, Legionnaires’ disease, Darwin, creationists, biologists, science, germ theory, microbe constancy, specificity, tuberculosis

Figure 1: Photograph of Dr. Robert Koch (1843–1910). Koch was the “father” of medical microbiology and is known for his many contributions to germ theory, bacteriology, and tropical medicine.3
Microbiology is dominated by evolution today. Just look at any text, journal article, or the topics presented at professional scientific meetings. Darwin is dominant. Many argue that “nothing in biology makes sense except in the light of evolution” (Dobzhansky 1973). But it was not always this way. In fact, a review of the major founders of microbiology has shown that they were creationists.1 We would argue that a better idea than evolution and one of much more practical importance is the germ theory of disease, originally put forth primarily by non-Darwinian biologists (Gillen and Oliver 2009). In our previous article (Gillen and Oliver 2009), we documented these and many other creation and Christian contributions to germ theory. But only recently has it become known that another important microbiology founder, Robert Koch (Fig. 1) and his co-workers were Linnaean creationists in their classification.2 This is due, in part, to additional works of Robert Koch that were translated from German to English. The year 2010 marks the 100th anniversary of his death (died: May 27, 1910). Although Koch and other German microbiologists were fairly secular in their thinking, their acceptance of Darwinian evolution was minimal.
As Dr. Henry Morris stated in The Biblical Basis of Modern Science, “The basic compatibility of science with Christian theism is obvious when it is realized that modern biology grew in large measure out of the seeds of such theism” (Morris 2002, p. 21). Christians, Jews, and non-religious scientists have contributed to the germ theory over the past 150 years. The basic history of the germ theory is given in many texts, most often giving credit to the experimental work of Louis Pasteur, Joseph Lister, and Koch. However, the role of worldview, and the fact that many were Christian and creation biologists, is often left out (Gillen and Oliver 2009). This article seeks to illustrate how creation principles of microbe constancy and specificity helped formulate and establish the germ theory. The successful application of the germ theory has saved millions of lives.
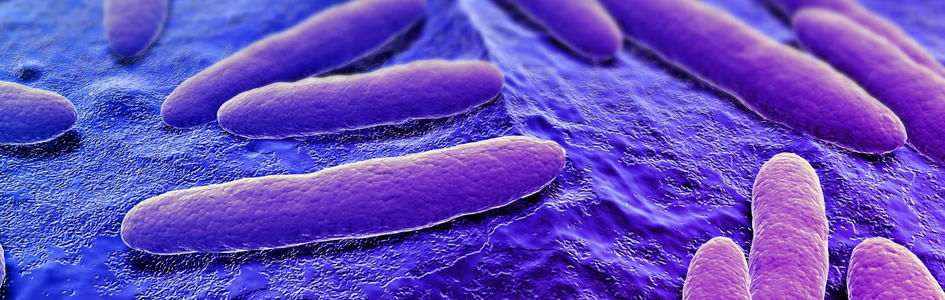
Most people are familiar with the tuberculosis (TB) skin test (also called the Mantoux TB skin test) taken prior to entering schools or the military. Koch discovered tuberculin4—a substance used in diagnosing TB that is now routinely used in TB screening tests. Tuberculin aids in manifesting an immune reaction (seen as a red wheal on the skin) to those that have been exposed to TB bacteria. Koch also succeeded in isolating the dreaded anthrax bacteria (Fig. 2), becoming the first to prove that a specific microbe caused a specific disease. From this classic study Koch developed four critical rules—still in use today—relating one kind of bacterium to one kind of disease. Virtually every student in introductory microbiology classes worldwide memorizes Koch’s postulates—the “rules” for determining cause and effect of infectious disease (Brock 1999).
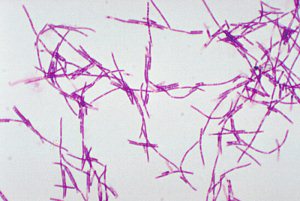
Figure 2: Photograph of Bacillus anthracis, the cause of anthrax.3
Robert Koch is most known for his development of rules, or postulates that determine the specific agent of infectious disease. His name is well known as one of the founders of medical microbiology. However, only a few people know about his knowledge of natural history and his Linnaean (creationist) classification of microbes. Koch and a number of other famous 19th century German microbiologists were very skeptical of Darwinian principles of classification, “transformation,” “transmutation,” and “spontaneous generation” as it related to microbes. In this article, we would like to show how the historic, Judeo-Christian worldview of creation and Linnaean classification played an important role in hygiene and applications of the germ theory of disease. In doing so, we continue a theme presented in earlier articles (Gillen and Sherwin 2008; Gillen and Oliver 2009).
Robert Koch and His Legacy
Dr. Robert Koch (1843–1910) received the Nobel Prize in Physiology and Medicine in 1905 “for his investigations and discoveries in relation to tuberculosis.” In that year, he was also recognized for demonstrating that specific bacteria can cause common diseases. Tuberculosis was the specific disease mentioned in the Nobel Prize, but Koch was already known for many other accomplishments in microbiology and tropical medicine. Koch is recognized as one of the founders of medical microbiology, the others being Pasteur and Lister. All of them were creationists. One of his co-workers and young colleagues, Paul Ehrlich (a Bible-believing Jew), won the Nobel Prize three years after Koch. Another young colleague, Emil von Behring won the first Nobel Prize in 1901 for his work on antibodies.
Robert Koch’s precision in his methodology and logic were valuable in finding the best technique for every specific case, such as providing special nutrient agar to maximize the growth for particular bacteria. Koch’s genius blazed new paths and gave present-day microbiology research its form. Koch’s methods helped creation microbiologist Carl Fliersman discover the cause of Legionnaires’ disease. Koch’s postulates were enhanced by his workers, Walther and Fannie Hesse, when they discovered a solid nutrient medium called agar. The solid medium allowed each individual microorganism present to develop into a fixed colony making it easier to obtain pure cultures of bacteria.
Shortly after the publication of his investigations into diseases from wound infections, Koch was appointed to the new hygienic institution, the Department of Health in Berlin. There he started work on some of the most important human diseases—namely, tuberculosis, diphtheria, and typhus. He worked on these investigations with his pupils and assistants, Friedrich Loeffler and Georg Gaffky. For all three diseases the specific bacteria were discovered and studied in detail. Koch started, or accomplished through his students, the major techniques used in medical microbiology. They would build upon the foundation of Pasteur and Lister. As the head of the German Hygiene Commission, Koch investigated the etiology of Asiatic cholera and discovered Vibrio cholera and the conditions necessary for its disease transmission. Koch and his co-workers found practical application in the development of measures taken to prevent and combat cholera in Egypt and India.
Koch perfected methods of isolating, culturing, and identifying bacteria. He was able to investigate disinfectants and methods of disease prevention important for hygiene and give advice concerning the early detection and combating of epidemic diseases such as cholera, typhus and malaria. In addition Koch conducted important investigations of malaria, tropical dysentery, African sleeping sickness, bubonic plague, and the Egyptian eye disease (trachoma). He also tackled typhus recurrens seen in tropical Africa. Koch conducted work of critical importance concerning a number of tropical cattle diseases, such as rinderpest (known as cattle plague), Surra (a protozoan disease also found in horses), Texas fever, Rhodesian red water fever, and the well-known African sleeping sickness (trypanosomiasis) transmitted by the tsetse fly.
Koch’s Early Studies on the Natural History of “Lower Forms of Plants”
Prior to his famous studies of anthrax and TB, Koch worked with Ferdinand Cohn (a botany expert in Germany) on the natural history of pigmented bacteria. (At the time, all bacteria were classified as plants—order Schizomycetes.) As a trained botanist, it was Cohn who first established the classification of bacteria according to Linnaean classification principles. In 1875, Cohn published this early classification of bacteria, starting with the genus Bacillus, and this eventually established bacteriology as a formal science (Gradman 2009).
During this same era, new ideas of evolution were creeping into biological classification systems, and some Darwinists were suggesting that out of a primordial soup bacteria evolved—and from them came “higher plants.” For example, Carl von Nägeli and other evolutionary biologists believed that bacteria could make dramatic mutations and easily change from one morphological type to another (cocci→bacilli→spirilla) in the supposed life cycle and evolution of shapes, which they called “pleomorphism.” Koch and Cohn did not believe in “intermediate forms”—missing links in the supposed evolution of microbes. They saw prokaryotes and protozoa as distinct and separate organisms and clearly understood their different life stages. This included vegetative cell and endospore formation in bacteria. They investigated protozoan parasites such as Plasmodium (malaria) and its different life stages. They had the experimental evidence to back their claims, whereas the “new” Darwinists were speculating on what might have happened.
Cohn and Koch, on the basis of their improved methodology and experience with pure cultures, defended the view of monomorphism. Monomorphism states that the morphological and physiological traits of bacteria are constant, stable, and can serve for identification and classification. Nägeli proposed that there must be intermediate forms of bacteria—life-forms in between observable bacteria. Some of the earlier studies done by Cohn were done on pigmented microbes—both algae and bacteria. Nägeli suggested that one form of microbe could transform or transmutate (evolve into another kind). In particular he suggested that micrococci (small, round bacteria) could become bacilli (rod-shaped bacteria) (Gradman 2009; Mazumdar (2002).
Koch completed some natural history studies with red pigmented bacteria on potato slices as agar was not yet used in microbiology studies. He called the bacteria Micrococcus prodigious. Although he could isolate both micrococci (probably Micrococcus roseus) and rods (probably Serratia marcescens) separately, one bacteria never transformed into the other. Koch now verified Cohn’s work that there were two distinct kinds of pigmented bacteria and one never transformed into another (Gradman 2009; Mazumdar 2002). These are both red bacteria, but very distinct and separate kinds of “lower forms of plants.”
Anthrax
After this, his early studies on the natural history of bacteria and learning from Cohn, Koch began to work on anthrax. According to Mazumdar (2002, p. 65) in his book, Species and Specificity, the anthrax bacillus was the first and major case for Koch’s argument of the constancy of microbes and their specificity in infectious disease. Dr. Koch’s classification and natural history of Bacillus anthracis was documented in photomicrographs. During his studies on the natural history of B. anthracis, Koch also observed and documented anthrax spores. He saw spores as further evidence of stability and constancy of species—a conservation of types (or kinds). According to one major review of Koch and anthrax:
“We must fix things, at least in a preliminary way, says Koch, and photographs are an excellent way to do it. They will get rid of numerous wilde Schössling, shots into the air. Koch points out that this [photograph of bacteria in sheep’s blood] shows four types of micrococcus, with no intermediate forms. . . . Koch comments that if the bacteria are left in their natural arrangement and not mixed up, no intermediate forms appear. . . . [He then shows a] group of mixed B. anthracis and B. subtilis, which form long threads. . . . B. anthracis shows spotting with light spots [when stained]; Koch notes that this distinguishes it from B. subtilis, which otherwise looks very like it. They differ not only physiologically, but also in appearance – they are quite different organisms. . . . Koch says these two photographs [of different types of bacteria] allow him to remark on Nägeli’s claim [evolutionary biologist and Koch rival] that staff shapes and threads are made by joining bacilli and spirilli, and that bacilli will break upon into micrococci [via transformation]. He emphasizes that he has been keeping his eyes open for this from the beginning and has never seen it. This is a matter of principle that must be solved if bacteriology is to get into a firm footing: bacteriology stands or falls on its truth or falsity. His experience, says Koch contradicts Nägeli’s” (Mazumdar 2002, p. 65).
During the last half of the 1800s, bacteria were suspected of causing numerous diseases. Men like Pasteur and Lister provided increasing evidence that bacteria caused infectious diseases such as anthrax, yet they could not provide the conclusive evidence. During this time anthrax ravaged European livestock, especially sheep. In some fields more than 10% of the sheep were lost. Since sheep were vital to Germany’s economy, an anthrax cure was paramount. Soon, both Koch and Pasteur concluded anthrax was caused by the bacterium B. anthracis (Fig.2).
Koch worked in a makeshift lab out of his home and used wild mice captured in his barn. He injected them with the blood of diseased sheep and cattle. He then performed autopsies and noted similar symptoms in mice that he had seen in sheep and cattle. Koch succeeded in isolating the bacillus but was unable to grow the bacteria on sterile media (potato slices or gelatin). He finally decided to grow the bacillus on the aqueous humor from the eyes of oxen. Koch could then observe the bacilli multiply, forming tangled threads and occasionally sporulation (producing spores). After inoculating animals with bacilli from the oxen’s aqueous humor, anthrax symptoms would appear in a day. Post mortem examination revealed the characteristic anthrax bacillus. As predicted, Jacob Henle’s (Koch’s mentor) postulates were satisfied—the cycle was complete. Koch took B. anthracis from a mouse, grew it in oxen aqueous humor, and then injected it into another mouse. He did this for 20 generations of mice to demonstrate that B. anthracis caused anthrax.
In addition, he tried injecting Bacillus subtilis (the hay bacillus), a similar yet distinct species, to show that it did not cause anthrax (Waller 2002, p. 109). Koch did this because Nägeli and Thomas Huxley claimed bacteria could somehow transform (evolve) from one species into another. Koch (a priori) did not agree and tested his hypothesis of bacteria being stable, constant, and highly specific. He found, after several generations of testing, that B. subtilis did not change (Waller 2002). This is an example of the logical nature of creation thinking leading to a breakthrough in germ theory and medicine. After 20 generations in mice, B. anthracis faithfully reproduced B. anthracis after its kind. In addition, he attempted to grow other spore-producing bacteria (such as B. subtilis) in mice, but they did not produce anthrax. He also documented the unique physiological properties of B. subtilis (Gradmann 2009; Waller, 2002). The bacteria did not change into other species of bacteria. Koch concluded that specific bacteria caused specific and characteristic infections. From early observations that B. anthracis was somehow implicated in anthrax came the final proof of it being the causative agent via elegant experiments in 1876. This finding was solidified by research done with Cohn in the late 1870s and 1880s. Modern evolutionary biologists acknowledge there are limits to observable changes in bacteria. According to Gophna (2009, p. 549), “despite lateral gene transfers, bacteria genera remain distinct, suggesting limits to gene flow between species.”
Koch’s Postulates and Anthrax
For the first time, these experimental methods enabled Koch and his co-workers to isolate specific bacteria and achieve a pure culture for suspected pathogens. They laid the groundwork for Koch to develop a logical series of observations and experiments that would prove the specific agent of an infectious disease. The series of steps worked out by Koch and others have become known as Koch’s postulates.
Koch’s work with B. anthracis provided absolute proof of the microbial etiology (cause) of an important infectious disease. Moreover, he enunciated a valuable principle. Fulfilling Koch’s postulates provides absolute proof that a particular microorganism causes a particular disease:
- The causative microorganism must be present in every individual with the disease.
- The causative microorganism must be isolated and grown in pure culture.
- The pure culture must cause the disease when inoculated into an experimental animal.
- The causative microorganism must be re-isolated from the experimental animal and re-identified in pure culture.
These four “rules” were a landmark in medical microbiology because they could be used to prove beyond a doubt that a particular bacteria was the cause of an infectious disease; not the mere association. Some bacteria may have been the result of a disease; not its cause (Brock 1961; Brock 1999).
Tuberculosis
Koch completed these famous postulates while studying anthrax, but the disease that made him famous was tuberculosis. TB is a lung disease consuming alveoli and other neighboring tissues. Around the turn of the 20th century, it was the leading cause of death worldwide. In the early 1880s, Robert Koch was working with the bacterium Mycobacterium tuberculosis (Fig. 3). This organism was of great interest because researchers suspected it caused the widespread, often-lethal infection. Koch made two important discoveries. He found a way of staining human tissue for microscopic examination that showed M. tuberculosis cells as thin blue rods on a brown background of human cells. He also found that M. tuberculosis—a slow-growing, highly fastidious bacterium—would grow on coagulated blood serum. With these tools, Koch set out to prove that tuberculosis was caused by M. tuberculosis (Brock 1961; Brock 1999).

Figure 4: A German Zeiss microscope (c. 1909) similar to the one used in Koch’s lab.6
Koch began by examining tuberculosis patients for the presence of M. tuberculosis. He found the bacterium in every patient—blue rods against brown tissue. Then Koch cultured the tuberculosis cells on coagulated blood serum, isolating pure M. tuberculosis cultures that he then injected into guinea pigs; they later succumbed to tuberculosis. M. tuberculosis could be cultured from guinea pigs; this fulfilled Koch’s 4th postulate. Unequivocally, M. tuberculosis caused tuberculosis.
Of course, Koch’s postulates cannot be met if the pathogen cannot be grown without infecting humans. Koch himself faced this dilemma later in his career while studying cholera. He discovered that a batch of V. cholera was present in all the intestines from all the patients he examined, and he was able to culture the organism from the guts. But he could not find an experimental animal susceptible to the disease. The third postulate was ultimately fulfilled when a physician working with Koch accidentally swallowed cholera bacteria and developed the disease. Koch’s postulates are not the only route to determining infectious etiology. They are, however, the best time-tested models for determining specific cause and effect in microbiology and parasitology even today.

Figure 5: A German Leitz microscope (c. 1910) similar to the one used in Koch’s lab.6
One reason that Koch was so successful in studying bacteria (and later tropical parasites) was his skill and innovations in microscope lenses. Not only did he use the best microscopes of his day, he also pioneered a partnership with Carl Zeiss and Ernst Abbe for microscope improvements. Koch visited Ernst Abbe for an exchange of ideas for improving the resolution for viewing bacteria. This meeting resulted in an oil immersion objective lens with a high resolving power and was introduced by Zeiss, the German microscope company. Another German microscope company, Leitz, also made high quality microscopes and had Koch test them. Koch became the “beta-tester” for both Zeiss (Fig. 4) and Leitz microscopes (Fig. 5). He used them in his microbiology and parasitology studies. These microscope brands had the best lens and illumination systems at the turn of the century.
Specificity Leads to Precise Diagnosis and Treatment in Malaria
Although Koch is most famous for his studies in bacteriology of anthrax, TB, and cholera (especially tuberculosis for which he received the Nobel Prize), he actually published more papers about tropical medicine. He made significant progress in treating two life-threatening parasitic protozoan, blood diseases—malaria and African sleeping sickness. He used quinine effectively against Plasmodium falciparum, the cause of malignant malaria and atoxyl against Trypanosoma brucei, the cause of African sleeping sickness. (Malignant malaria is the common name given to malaria caused by Plasmodium falciparum).
Malaria is an acutely parasitic disease caused by protozoa of the genus Plasmodium and transmitted from human to human only by Anopheles mosquitoes. It is one of the most common and widespread of all parasitic diseases. It would not be an exaggeration to call it the most prevalent parasitic disease now suffered by humans. Malaria is frequent and severe in tropical and subtropical countries, but occurs in localized endemic areas throughout most of the world. The disease is annually responsible for an estimated 1 million deaths among children. Perhaps one in every 10 people worldwide has had the disease sometime during their life.
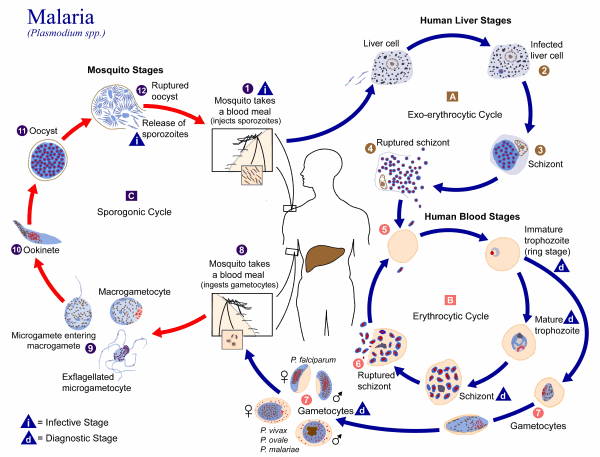
Click image to enlarge.
Figure 6: Life cycle of the parasites of the Plasmodium, causal agents of malaria. Also, Koch treating the disease with quinine.7
All species of malaria organisms pass through the same life cycle. Plasmodium has a complex life cycle involving transmission between several hosts. This complex life cycle makes it difficult to develop a vaccine. There are two distinct phases: in the mosquito, where Plasmodium undergoes sexual reproduction; and in the human body, where Plasmodium undergoes asexual reproduction. A diagram summarizing the life cycle is given in Figure 6. The life cycles of the malarial parasites have three important stages: the sporozoite, the merozoite, and the gametocyte. Each is a factor in malaria. The mosquito sucks human blood and acquires gametocytes, the form of the protozoan found in red blood cells (Gillen 2007, p. 59).
Koch was successful in treating patients with malaria using quinine; whereas its prior use had limited success. Why? He understood the life stages of the malaria parasite. In addition, his creationist view of species and specificity of parasites held for life stages, as well as created kinds. In other words, there were predictable patterns that did not vary and that drugs specific to life form stages would be most effective.
Quinine had been the “miracle drug” of the day; however, it did not always work. It was frequently used at the wrong stage of malaria and sometimes made things worse. Many physicians only applied quinine when there was an active infection. Those cases that were latent—showing no symptoms at all—were not treated. As a result some people who had latent infections would develop Blackwater fever. Blackwater fever is a grave condition associated with malignant malaria, but its clinical picture is distinct. It is an acute, massive lysis of red blood cells marked by high levels of hemoglobin and waste products in blood and urine. The urine is a very deep dark red color and an indication of renal failure. In recent years, it has declined dramatically due to the use of quinine for prophylaxis—Koch’s idea!
Koch’s work on malaria was the result of his detailed diagnosis of blood samples. By observing blood cells, Koch could not only tell if a patient had malaria, but also at what stage. For example, Koch could tell if patients had “latent” malaria—an ongoing infection without clinical symptoms. In addition, he could tell how much of the drug to administer to a patient based upon the stage of malaria and its “load.” He could give just the right amount of quinine and later check the progress of the infection by re-checking the blood for the Plasmodium parasite (Knight 1961, pp. 126–127).
A vivid proof of the success of Koch’s method came in 1900. In Brioni, an island in the Adriatic Sea, about 300 people were threatened with malignant malaria (probably P. falciparum). All 300 were tested, but only 22% actually had the serious form. After diagnosis, Koch administered quinine in precisely the right amount and saved them from almost inevitable death if not treated. In honor of this great success, the island erected a statue of his likeness (Knight 1961, pp. 126–127).
Koch studied the protozoan parasite Trypanosoma, which—like malaria—is also found in the blood and spread by an arthropod. He understood that Trypanosoma brucei had variations in the wide African continent. One species of Trypanosoma only infected cattle (Nagana), while other species caused East and West African sleeping sickness in people. Koch understood its variation and subspecies in Africa; he did not see it as a contradiction of his rejection of transformation from one protozoan type into another. He did understand variation within a protozoan kind. He had limited success in finding treatment for African sleeping sickness with atoxyl, but also found it could be toxic.
The “Germ Men” Living a Century Ago
The study of microbial pathogenesis—the relationship between pathogenic microorganisms and the diseases they cause—began a little more than 100 years ago, when Koch conclusively proved that a specific species of bacterium caused a specific human disease. Koch’s success, along with Pasteur’s at about the same time, initiated a period of intense research. This period—from the late 1800s through the early 1900s—became known as the Golden Age of Microbiology. Most major bacterial pathogens were isolated during this time. The techniques were fairly basic: isolate the microorganism, grow it in pure culture, and examine human and microbial cells under the microscope. Koch influenced many students, most of which were Linnaean botanists/microbiologists (i.e., each of them had a limited view of “evolution,” rejecting most of Darwinism while accepting a degree of natural selection). Even today, the term “Linnaean” refers to “a hierarchical system of fixed categories,” emphasizing overall separate, fixed kinds (i.e. taxonomic families) of living things, but allowing for variation within those kinds via mechanisms like natural selection.
Koch started a hygiene institute in Berlin, and out of it came many great microbiologists, including Emil Von Behring, Richard Pfeiffer, Friedrich Loeffler, and Paul Ehrlich. These were the “apostles” of germ theory. As a result of their influence (along with Pasteur and Lister), a “gospel of germs” spread to the USA and health practices began to change (Bulloch 1938).
Koch and co-workers held a view that was consistent with the Old Testament view of disease. The idea of specificity in diagnosing infectious skin disease (then called “leprosy” or contagion) appears to have its roots in the Bible. We read of many specific symptoms in the Levitical law and then a pronouncement of clean or unclean. The diagnosis and “treatment” was prescribed by the Levites, who served as public health servants, or physicians, in that day.
Regulations about Infectious Skin Diseases
The LORD said to Moses and Aaron, “When anyone has a swelling or a rash or a bright spot on his skin that may become an infectious skin disease, he must be brought to Aaron the priest or to one of his sons who is a priest. The priest is to examine the sore on his skin, and if the hair in the sore has turned white and the sore appears to be more than skin deep, it is an infectious skin disease. When the priest examines him, he shall pronounce him ceremonially unclean. If the spot on his skin is white but does not appear to be more than skin deep and the hair in it has not turned white, the priest is to put the infected person in isolation for seven days. On the seventh day the priest is to examine him, and if he sees that the sore is unchanged and has not spread in the skin, he is to keep him in isolation another seven days. On the seventh day the priest is to examine him again, and if the sore has faded and has not spread in the skin, the priest shall pronounce him clean; it is only a rash. The man must wash his clothes, and he will be clean. But if the rash does spread in his skin after he has shown himself to the priest to be pronounced clean, he must appear before the priest again. The priest is to examine him, and if the rash has spread in the skin, he shall pronounce him unclean; it is an infectious disease.” Lev. 13:1–8 (NIV)
Koch believed in the idea of specificity of diagnosis and applied it to present day infections and later parasites. Although Koch was never associated with “religion” or church, he was baptized as an infant in the Lutheran church and did have formal religion classes when he was young. Also, there was the influence of Cohn (his mentor in the natural history of bacteria) and his young colleague, Ehrlich (who pioneered a remedy for syphilis), who were both orthodox Jews and seem to have been religious and familiar with the Bible.
Koch’s Postulates Applied Today
In 1876–77, Dr. Robert Koch solved the mystery of what caused anthrax. In 1976–77, Dr. Carl Fliermans, a modern creationist, helped solve the mystery of Legionnaires’ disease using Koch’s postulates. In July 1976, a mysterious illness struck hundreds of veterans with an unusual life-threatening pneumonia. It became a national focus of an intense investigation that resulted in the discovery in January 1977 of a Gram-negative, rod-shaped bacterium that was found to cause the disease. The bacterium was named Legionella pneumophila. Almost 100 years after the discovery of anthrax, a new problem arose in the USA. In one of the most dramatic entrances of any disease into the public-health arena, Legionnaires’ disease appeared at the U.S. Bicentennial Convention of the American Legion, July 1976, in Philadelphia. Nearly 5,000 Legionnaires attended the three-day meeting, with over 600 staying at the elegant but aging Bellevue Stratford Hotel. Even before checking out of the hotel, several Legionnaires began to feel ill with flu-like symptoms. On Tuesday, July 27, only four days after leaving Philadelphia, an Air Force veteran who had stayed at the Bellevue Stratford during the convention died at a hospital in Sayre, Pennsylvania. He was the first of more than 30 Legionnaires to eventually succumb to a lethal pneumonia that the news media quickly named “Legionnaires’ disease.” What was the cause of this new disease? It would take the Centers for Disease Control (headed by Dr. Joseph McDade) to isolate a new organism, Legionella pneumophila. But, the CDC with hundreds of workers could not complete Koch’s postulates to prove that the new found bacterium was the cause. McDade asked Dr. Carl Fliermans to help in the investigation (Gillen 2007).
In the spring and summer of 1977 Fliermans described the ecology of the Legionella bacteria. He was a microbial ecologist with DuPont and was on the technical advisory board at the Institute for Creation Research at that time in San Diego. Fliermans was the scientist who painstakingly and successfully isolated the causative agent of Legionnaires’ disease. He is a Christian who credits the Creator for guiding him in his discovery of Legionella. Good microbiologists like McDade and Fliermans considered pathogenic sources in nature, routes of transmission to susceptible persons, and means of preventing the spread of pathogens. Their process illustrates how classical techniques are used to prove and/or implicate the cause of a specific disease.
Since 1969, Fliermans had been conducting fascinating research on microorganisms found within thermal habitats, such as those at Yellowstone and thermal streams from man-made habitats. The bacteria associated with these hot water habitats were often associated with an optimal growth temperature between 30º and 90ºC. These “thermopiles” (heat-lovers) were just like the clinical isolates of Legionella. Armed with this information, Fliermans began looking in other aquatic habitats for the presence of Legionella. He found them living symbiotically in warm waters with freshwater amoebas and algae. For Fliermans, the question now became: how and where does Legionella fit in the ecological setting?
Many at the CDC were puzzled regarding the origin of Legionella. But the epidemiological data led Fliermans to focus on aquatic niches as the bacterium's natural habitats. He was aware that some infections had been associated with people who had stayed in hotels that had old air conditioning systems. Legionella was found growing inside damp pipes that heated to 125–150ºF in the hotel’s AC system. A biofilm (consisting of a mixture of algae, amoebas, and bacteria) coated the inside of the pipes and Legionella bacteria that grew in the biofilm became aerosolized in droplets and were carried through the AC system and infected people. Clinical data indicated a seasonality of infection that fit well with the use of the AC system. Such a cyclic pattern was very similar to that observed for the growth of aquatic bacteria.
Click image to enlarge.
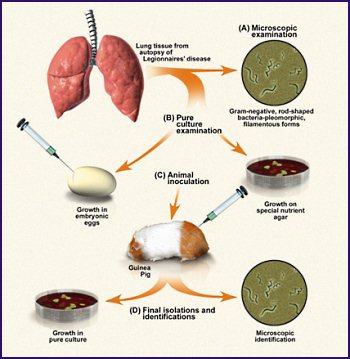
Figure 7: The investigation of Legionnaires’ disease by Fliermans and his use of Koch’s postulates.8
Figure 7 traces the investigation of the etiology of Legionnaires’ disease and summarizes Koch’s postulates. Legionnaires’ disease was first recognized in July 1976. It was more than six months later before Koch’s postulates were fulfilled and L. pneumophila was pronounced the etiologic agent of the disease. First, if the etiological agent were biological, then the agent had to be found to be regularly associated with the disease. Tissues from lung biopsies and sputum samples were examined for a recurring microorganism. A Gram-negative rod with a tendency to form long, looping filaments was consistently detected in specimens. Second, the newly discovered bacterium was isolated in pure culture in the laboratory. This necessitated investigating L. pneumophila’s nutritional requirements and designing special growth media that would meet these narrow requirements for bacterial growth. Third, a susceptible animal was needed to demonstrate that L. pneumophila could produce disease, particularly a respiratory disease similar to Legionnaires’ disease in humans. The guinea pig was that animal. L. pneumophila was recovered from infected guinea pigs fulfilling Koch’s fourth postulate (Fig. 7).
Summary of Robert Koch’s Work
In summary, Koch was a master of operational science but a skeptic of Darwinian evolution. Thomas Brock (1999, p. 286) says of Koch: “Koch was one of the most influential and dedicated medical researchers of the nineteen century.” His motto, nunquam otiosus (never idle) expressed the essence of his life. His close friend and colleague, Ehrlich, placed him among the “princes of medical science” and thought that Koch was an experimenter par excellence. Ehrlich also stated about Koch that “Careful and patient observation, hard work and keen insight were the tools of his trade” (Brock 1999, pp. 286–287). Koch provided evidence or proof for the causative agents of anthrax, TB, and cholera. He also did extensive studies on malaria, African sleeping sickness, and many other tropical diseases that had plagued both humans and animals. In fact, he completed more papers on tropical, parasitic diseases than his more famous papers on bacteriology.
Koch approached his first major work, the life cycle of B. anthracis and B. subtilis as a problem in natural history, but he quickly discovered the practical significance of his work and went on (along with Pasteur) to help control the disease. Although there was a marked contrast between French and the German approaches to infectious disease, they were complimentary (Brock 1999). Pasteur and the French developed treatments for individuals, whereas, Koch and the Germans developed approaches for the control of infectious disease in populations. Koch emphasized specificity in the cause of infectious diseases; Pasteur emphasized variation of virulence within a kind. Both were creationists: Pasteur was religious; Koch was not. Pasteur was very public in his appeal and sometimes theoretical in his ideas, lacking the “final proofs.” Koch was private and usually emphasized precision. On occasion they cooperated, but, more often, they competed. They did have a common friend, Christian and creationist Joseph Lister. All three were giants in microbiology and founders of a new field of medicine.
Koch was rigid in views, but he was right most of the time. He believed in the monomorphic nature of bacteria (minimal variation); Pasteur saw bacteria having greater variation in virulence than Koch (such as anthrax bacillus that could be rendered nonpathogenic by heating it). Both saw discontinuity in bacterial forms. Conversely, Nägeli, Darwin, and Huxley believed in a continuous line of bacteria life-forms from “simple” to complex (molecules-to-man evolution). These three men also believed in “transformation” of one microbial type into another (such as coccus or bacillus species changing into spirilla species).
After Koch opened the way, other microbiologists and physicians discovered other specific disease-causing germs. The contributions of creationists Pasteur and Lister had paved the way for proof of the germ theory of disease. The application of Koch’s postulates in discovering the specific agent in disease would mark the pinnacle of the Golden Age of Microbiology. Many bacteriologists consider 1876 to be the year medical microbiology became a valid scientific discipline. Good science is marked by careful observation, repeatability of experiments, falsifiability, and predictive power. Koch’s postulates’ demand for proof of cause and effect provided epidemiologists and physicians a framework with which to diagnose and treat infectious and parasitic diseases.
Thomas Brock (1999) says of Koch: “Religion never entered his life.” It should be pointed out that it is very unlikely that Koch was a Christian. He was baptized as an infant (Lutheran) but was never considered to be religious nor did he attend church as an adult. He basically had no interest in “religion” and did not comment on it. He did embrace a creation classification system, which is why we have written the article. His early teaching on “religion” as a school boy and/or the influence of orthodox Jewish friends (Cohn and Ehrlich) may have something to do with his traditional view of classification and view of natural history (Bulloch 1938).
Creation Thinking Leads to Better Medicine
Since the Fall, man has struggled to conquer disease, one of the curses brought upon by sin. But only in the past century has humanity made significant strides toward curing and preventing these scourges. Today there is a failure of scientists to recognize and acknowledge the clear evidence of the Creator’s hand in the world around us (Romans 1:20). This was not the case just a century ago. There were a number of Christian and creation biologists that were founders of tropical medicine and involved in the discovery of microorganisms, vectors, and parasites (Graves 1999). Some notable scientists were either traditional Catholics or evangelical Christians (Gillen and Oliver 2009). In addition to Koch, almost the entire school of “Germ Men” of the 19th century was composed of Linnaean creationists. Their lives were focused on experimental science as it related to infectious disease, but they were also influenced by a Judeo-Christian worldview of origins.
Today, evolutionary ideas are prominent in microbiology. Most secular biologists claim antibiotic resistance in bacteria as an example of “evolution in action,” when it really isn’t (Purdom 2007). This seems to be the majority opinion among professional biologists. They want to link On the Origin of Species by Means of Natural Selection (Darwin 1859) with the origin of microbes from inorganic matter. Fortunately, the idea of biogenesis was proven by Pasteur, Lister, and Koch. Each of these men rejected evolution as Darwin proposed it. They accepted natural selection, and perhaps today they would embrace natural selection happening with antibiotic resistance. Yet, this is not evolution in action; it is simply variation and a type of artificial selection.
Most of the founders of modern-day microbiology and parasitology held a worldview that was consistent with historic and traditional biblical teachings, including Creation, Corruption, Curse, and Christ. There is no question that Christians and non-Christians have clearly added to the modern-day germ theory of disease. But, sadly, today there are very few creation microbiologists within these ranks. The good news is that a group of modern-day creation microbiologists are emerging from the Microbe Forum (Purdom and Francis 2008), sponsored by Answers in Genesis. The forum’s purpose is to present creation research on the role of microbes in the world. With a possible resurgence of the God-honoring biblical worldview, science might again be blessed with more medical discoveries that would increase humanity’s quality of life (Mitchell 2005).
Acknowledgements
We would like to express our appreciation to Dr. Paul Sattler for taking photographs of the microscopes. We wish to also thank Dr. Georgia Purdom for all her comments and providing feedback on earlier drafts of the manuscript.
References
Brock, T. 1961. Milestones in microbiology. (pp. 69 - 75). Washington DC: The American Microbiology Society.
Brock, T. D. 1999. Robert Koch: A life in medicine and bacteriology. Washington DC: The American Microbiology Society.
Bulloch, W., 1938. The history of bacteriology, New York: Dover Publications.
Darwin, C. 1859. On The Origin of Species By Means of Natural Selection. London: John Murray.
Dobzhansky, T. 1973. Nothing in biology makes sense except in the light of evolution. The American Biology Teacher 3:125-129.
Gillen, A. L. 2007. The Genesis of Germs: Disease and the Coming Plagues in a Fallen World, Green Forest, AR: Master Books.
Gillen, A. L. and F. Sherwin, 2008. Louis Pasteur’s Views on Creation, Evolution, and the Genesis of Germs. Answers Research Journal (1): 43–52.
Gillen, A. L. and Oliver, J. D. 2009. Creation and the Germ Theory: How a Biblical Worldview Helped Shape the View that Germs Make Us Sick. Answers in Genesis, Answers In-Depth, July 29, 2009 posted.
Graves, D. 1999. Doctors who followed Christ. Grand Rapids, MI: Kregel Publications.
Gophna, U. 2009. Complexity apparently is not a barrier to lateral gene transfers. Microbe Magazine 4 (12), pp. 549-553.
Gradmann, C. 2009. Laboratory disease: Robert Koch's Medical Bacteriology. Baltimore, MD The Johns Hopkins University Press.
Knight, D. C. 1961. Robert Koch: Father of Bacteriology (Immortals of Science Series) New York. Franklin Watts, Incorporated.
Mazumdar, P. M. H. 2002. Species and Specificity: An Interpretation of the History of Immunology. Cambridge, United Kingdom. Cambridge University Press.
Mitchell, R. T. 2005. Evolution and medicine. https://answersingenesis.org/natural-selection/antibiotic-resistance/evolution-and-medicine/ (posted November 22, 2005).
Purdom, G. 2007. “Antibiotic Resistance of Bacteria: An Example of Evolution in Action?” Answers Magazine. http://www.answersingenesis.org/articles/am/v2/n3/antibiotic-resistance-of-bacteria
Purdom, G. and Francis, J. 2008. “Proceedings of the Microbe Forum, June, 2007” Answers Research Journal (2008): 1-6. http://www.answersingenesis.org/articles/arj/v1/n1/proceedings-microbe-forum
Waller, J. 2002. The Discovery of the Germ. New York, Columbia University Press.
Footnotes
- The term creation biologist is used in a broad sense. Although there is strong historical evidence that each of these men had a creation worldview, the exact stance of each (young-earth, old-earth, progressive creation) is not known. You can read more about this in the book The Genesis of Germs (Gillen 2007).
- Linnaean creationists—the term Linnaean refers to “a hierarchical system of fixed categories”; emphasizing overall separate, fixed kinds (i.e., taxonomic families) of living things but allowing for variation within those kinds.
- Taken from: Wikimedia Commons, http://commons.wikimedia.org/wiki/Main_Page.
- Tuberculin is the name given to a Mycobacterium extract that is used in skin testing animals and humans to identify a tuberculosis infection.
- CDC image, ID#:1064.
- Microscope from the personal collection of Alan Gillen.
- CDC image, ID#:3405.
- Diagram taken from The Genesis of Germs, p. 39 (Gillen 2007).

Answers in Genesis is an apologetics ministry, dedicated to helping Christians defend their faith and proclaim the good news of Jesus Christ.
- Customer Service 800.778.3390
- Available Monday–Friday | 9 AM–5 PM ET
- © 2026 Answers in Genesis