Chapter 3
Bacteria in a Fallen World
Section 1
Koch’s Postulates and TB
For several decades during the 1800s, bacteria were suspected of causing disease. Men like Pasteur and Lister had provided increasing evidence that specific bacteria caused certain diseases, like anthrax, yet they could not provide the conclusive evidence needed to prove the developing theory. They did, however, lay the groundwork for Robert Koch to develop a logical series of observations and experiments that would prove the specific element of infectious diseases. The series of steps worked out by Koch and others has become known as Koch’s postulates. He completed the famous postulates with anthrax, but the next important disease that made it famous was tuberculosis. TB is a lung disease consuming alveoli and other neighboring tissues. At the turn of the 20th century, it was the leading cause of death in the United States. It is still the number one killer worldwide; about two billion people (one-third of the world) test positive for antibodies against the bacterium causing TB.
In the early 1880s, Robert Koch was working with the bacterium Mycobacterium tuberculosis. The organism was of great interest because researchers suspected it caused the widespread, often-lethal infection. Koch made two important discoveries. He found a way of staining human tissue for microscopic examination that showed M. tuberculosis cells as thin blue rods on a brown background of human cells. He also found that M. tuberculosis —a slow-growing, highly fastidious bacterium—would grow on coagulated blood serum. With these tools, Koch set out to prove that tuberculosis was caused by M. tuberculosis. In the 1880s, not only was there no proven connection between the two, there was also no proof that any particular microorganism caused any particular disease.
Koch began by examining tuberculosis patients for the presence of M. tuberculosis cells. He found the bacterium in every patient—blue rods against brown tissue. Then Koch cultured the tuberculosis cells on coagulated blood serum, isolating pure M. tuberculosis cultures he injected into guinea pigs. They succumbed to tuberculosis. Unequivocally, M. tuberculosis caused tuberculosis. Koch’s work with M. tuberculosis provided absolute proof of the microbial etiology (cause) of an important infectious disease. Moreover, he enunciated a valuable principle. Fulfilling Koch’s postulates provides absolute proof that a particular microorganism causes a particular disease:
- The causative microorganism must be present in every individual with the disease.
- The causative microorganism must be isolated and grown in pure culture.
- The pure culture must cause the disease when inoculated into an experimental animal.
- The causative microorganism must be re-isolated from the experimental animal and re-identified in pure culture.
Of course, Koch’s postulates cannot be met if there is no way the pathogen can be grown or if it only infects humans. Koch himself faced this dilemma later in his career when studying cholera. He discovered that a batch of Vibrio cholera was present in all the intestines from all the patients he examined and was able to culture the organism. But he could not find an experimental animal susceptible to the disease. The third postulate was ultimately fulfilled when a physician working with Koch accidentally swallowed cholera bacteria and developed the disease. Koch’s postulates are not the only route to determining infectious etiology. They are, however, the best time-tested models for determining specific cause and effect in bacteriology.
The study of microbial pathogenesis—the relationship between pathogenic microorganisms and the diseases they cause—began little more than 100 years ago, when Robert Koch conclusively proved that a specific species of bacterium caused a specific human disease. Koch’s success, along with Louis Pasteur’s at about the same time, initiated a period of intense research. This period—from the late 1800s through the early 1900s—became known as the Golden Age of Microbiology. Most major bacterial pathogens were isolated during this time. The techniques were fairly basic: isolate the microorganism, grow it in pure culture, and examine human and microbial cells under the microscope.
Until relatively recently, most of our knowledge about microbial virulence and pathogenesis was based on the same techniques. Clinicians observed the manifestations of a disease, pathologists examined diseased tissue grossly and under the microscope, and microbiologists used Koch’s postulates to prove that a given microorganism was the etiologic agent of a given disease. One character sketch of Dr. Robert Koch by Sir Arthur Conan Doyle (Review of Reviews, December 1890, p. 552) said:
Never, surely, could a man have found himself in a position less favorable for scientific research—poor, humble, unknown, isolated from sympathy and from the scientific appliances which are the necessary tools of the investigator. Yet he was a man of too strong a character to allow himself to be warped by the position in which he found himself or too diverted from the line of work which was most congenial to his nature.
| Date | Disease | Bacterium | Date | Disease | Bacterium |
|---|---|---|---|---|---|
| 1876 | Anthrax* | Bacillus anthracis | 1886 | Pneumonia | Streptococcus pneumoniae |
| 1879 | Gonorrhea | Neisseria gonorrhoeae | 1887 | Meningitis | Neisseria meningitidis |
| 1880 | Typhoid fever | Salmonella typhi | 1887 | Brucellosis | Brucella spp. |
| 1880 | Malaria | Plasmodium spp. | 1892 | Gas gangrene | Clostridium perfringens |
| 1881 | Wound sepsis | Staphylococcus aureus | 1894 | Plague | Yersinia pestis |
| 1882 | Tuberculosis* | Mycobacterium tuberculosis | 1896 | Botulism | Clostridium botulinum |
| 1883 | Cholera* | Vibrio cholerae | 1898 | Dysentery | Shigella dysenteriae |
| 1883 | Diphtheria | Corynebacterium diphtheriae | 1905 | Syphilis | Treponema pallidum |
| 1885 | Tetanus | Clostridium tetani | 1906 | Whooping cough | Bordetella pertussis |
| 1885 | Diarrhea | Escherichia coli | 1909 | Rocky Mountain spotted fever | Rickettsia rickettsii |
After Robert Koch opened the way for precise methodology in epidemiology, other microbiologists and physicians discovered other specific disease-causing germs. Table 3.3 lists the history of some of these discoveries. The contributions of creationists Louis Pasteur and Joseph Lister had paved the way for proof of the Germ Theory of Disease. The application of Koch’s Postulates in working out the specific element in disease would mark the pinnacle of the Golden Age of Microbiology. Many bacteriologists have considered 1876 to be the formal introduction of medical microbiology as a scientific subdiscipline. The importance of Koch’s Postulates lies in its demand for rigorous logical proof of cause and effect. Good science is marked by keen observation, repeatability of experiments, falsifiability, and predictive power. Koch’s Postulates provided epidemiologists and physicians with a framework to diagnose and treat infectious and parasitic diseases. If only more biology subdisciplines, like the study of origins, required such rigorous proofs before wild speculations about phylogenic trees, cladograms, and vestigial organs took place, the world of biology would be a better place. It is the observable evidence in biology, not evolution, that leads us to cause-and-effect relationships. Here’s how Carl Fliermans, a modern creationist and excellent microbiologist, investigated the cause of Legionnaire’s disease and fulfilled the requirements of Koch’s Postulates.
Creation Scientist Focus 3.1
Carl Fliermans and His Research on Legionella
Dr. Carl B. Fliermans is a microbial ecologist with DuPont and is on the technical advisory board at the Institute for Creation Research. He holds a Ph.D. in microbiology from Indiana University, and a post-doctoral fellowship at the National Institutes of Health. Dr. Fliermans is the scientist who first isolated the “Legionnaires’ Disease” bacterium. He has published over 60 works, and is a member of the American Society for the Advancement of Science, the American Institute for the Biological Sciences, and the American Society for Microbiology, among others. Dr. Fliermans is a Christian who believes the Creator guided him in his discovery of Legionella.
August 1976 Newspaper Headline: “Mystery Illness Strikes Legionnaires”
In one of the most dramatic entrances of any disease into the public-health arena, Legionnaires’ disease appeared at the U.S. Bicentennial Convention of the American Legion, July 21–23, 1976, in Philadelphia. Nearly 5,000 Legionnaires attended the three-day meeting, with over 600 staying at the elegant but aging Bellevue Stratford Hotel. Even before checking out of the hotel, several Legionnaires began to feel ill with flu-like symptoms. On Tuesday, July 27, only four days after leaving Philadelphia, an Air Force veteran who had stayed at the Bellevue Stratford during the convention died at a hospital in Sayre, PA. He was the first of more than 30 Legionnaires to eventually succumb to a lethal pneumonia that the news media quickly named “Legionnaires’ disease.” What was the cause of this new disease?
- Was it biological or chemical?
- Where did the pathogen, if there was one, come from?
- How was the disease spread?
- How could the disease be prevented?
These key questions and more became the focus of an intense investigation that resulted in the discovery in January 1977 that a Gram-negative, rod-shaped bacterium caused the disease. The bacterium was named Legionella pneumophila. Good microbiologists like Dr. Joseph McDade and later Dr. Fliermans considered pathogenic sources in nature, routes of transmission to susceptible persons, and means of preventing the spread of pathogens. Their process illustrates how classical techniques are used to prove the cause of a specific disease.
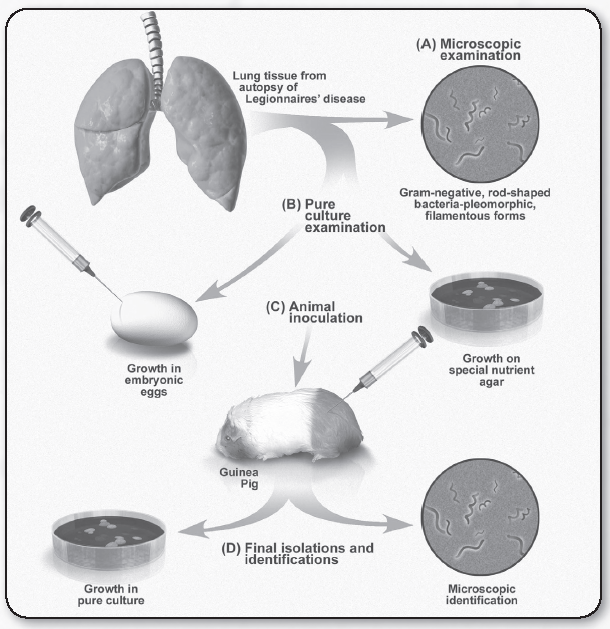
Investigation of the etiology of Legionnaires’ disease and summarizes Koch’s postulates.
The illustration above traces the investigation of the etiology of Legionnaires’ disease and summarizes Koch’s postulates. Legionnaires’ disease was first recognized in August 1976. It was more than six months before Koch’s postulates were fulfilled and Legionella pneumophila was pronounced the etiologic agent of the disease. First, if the etiological agent were biological, then the agent had to be found to be regularly associated with the disease. Tissues from lung biopsies and sputum samples were examined for a recurring microorganism. A Gram-negative rod with a tendency to form long, looping filaments was consistently detected in specimens. Second, the newly discovered bacterium was isolated in pure culture in the laboratory. This necessitated learning L. pneumophila’s nutritional requirements and designing special growth media that would meet these requirements, supporting the bacterium’s growth. Third, a susceptible animal was needed to demonstrate that L. pneumophila could produce disease, particularly a respiratory disease similar to Legionnaire’s disease in humans. The guinea pig proved to be the animal model of choice. Finally, L. pneumophila was recovered from infected guinea pigs to verify that it had established an infection.
Initial Isolation of Causative Agent
Through a series of experiments, Dr. McDade and his team first discovered from clinical specimens in January 1977 the evidence for the existence and pathogenesis of the bacterium that causes Legionnaires’ disease. The first step was to remove lung samples from a deceased Legionnaire. These cells were ground up, injected into chicken eggs, and incubated. After the incubation period, the eggs were cracked, and the yolk sacs extracted and injected into the footpads of guinea pigs. These animals then developed the typical symptoms of Legionnaires’ disease. McDade then drew blood samples from disease survivors, assuming they contained antibodies against the causative agent. He then mixed the samples with the yolk-sac isolates, and they reacted, confirming that the agent in the yolk sacs was the same agent causing disease in the 33 people.
McDade explained that his team had been stumped for months by several unusual characteristics of the bacteria: The bacteria did not grow under typical conditions. The scientists tried to culture the bacterium from the Legionnaires’ blood and tissue samples in a solution filled with standard media fluid used to grow other bacterial varieties. However, nothing grew. This lack of growth led the team to think that the agent was a virus or “Andromeda strain” never seen before. It was not until samples not treated with antibiotics were injected into the eggs that evidence of biological activity was determined.
Another delay was caused by the use of mice in experiments. It was not until the team switched to guinea pigs that their efforts were productive. Though mice are often used as animal models, it turned out that Legionella replicate primarily inside macrophages. Mice macrophages are very inefficient at ingesting this bacterium, so they never got infected from samples from the Legionnaires. In contrast, guinea pigs were susceptible to Legionella and got infected.
The next step for McDade was to determine why this bacterium was so difficult to culture. They soon discovered that the Legionella bacterium has physiological needs. Standard culture media does not promote growth because it requires high levels of the amino acid cysteine, inorganic iron supplements, low sodium concentrations, activated charcoal, and elevated temperatures. Dr. Fliermans was the first to recognize that the lipids of Legionella were very similar to the thermophilic bacteria he discovered in the thermal areas at Yellowstone National Park. Also, the bacterium tends to live in a nutrient-rich, dark environment as a biofilm (scum) associated with selected algae species. These conditions contributed to the difficulty in viewing the organism in its environment using standard microscopy and other techniques.
McDade asked Fliermans to help complete Koch’s postulates for Legionnaires’ disease. Since 1969, Fliermans has been conducting research on microorganisms associated with natural thermal habitats like those at Yellowstone and man-made habitats coming from thermal streams near electrical and nuclear facilities. The microorganisms associated with these habitats were often mesophilic and thermophilic in their physiological response in that their optimal growth temperature was between 30° and 90°C (86º and 194ºF). The second characteristic unusual for these thermophiles was the large number of branched-chained fatty acids they contained, just like the clinical isolates of Legionella. Armed with this information, Fliermans began looking in aquatic habitats, both natural and man-made, both ambient and thermal, for the presence of Legionella. Fliermans’ seminal work demonstrated that Legionella could be isolated from natural habitats not associated with an outbreak of the disease. These findings opened a new area for thinking, experimentation, and understanding. For Fliermans, the question now became: How and where does Legionella fit in the ecological setting?
Although many at the Centers for Disease Control were puzzled as to the origin of Legionella, the epidemiological data lead Fliermans to focus on aquatic niches as the bacterium’s natural habitats. This hypothesis came from examining the fact that initial clinical presentations demonstrated a seasonality of infection. Such a cyclic pattern was very similar to that observed for the growth of aquatic bacteria. Theories as to the cause of the illnesses ranged from nickel carbonyl intoxication and viral pneumonia to a pharmaceutical conspiracy against American veterans. At the CDC, many hypothesized that Legionella may have been genetically engineered as an “Andromeda strain” by the Soviets or as some other Communist plot. After all, it had primarily affected veterans. Reading his Bible one day, Dr. Fliermans observed Ecclesiastes 1:9: “The thing that hath been, it is that which shall be; and that which is done, is that which shall be done: and there is no new thing under the sun.” Dr. Fliermans believed this was true, and soon altered the way his laboratory looked for the organism, since the bacterium was probably not new under the sun. After praying, planning, and exploring, Dr. Fliermans found the bacterium in thermal waters (initially isolated at 45°C [113ºF] at Savannah River Laboratory) discharged from a nuclear reactor and subsequently from natural hot springs in both the Eastern and Western United States. Once isolated from the environment, the next task was to culture it. At first, it grew only in guinea pigs. Koch’s postulates were initially fulfilled in Dr. Fliermans’ daughter’s guinea pig in the summer of 1977 with samples drawn from cooling towers. He was able to develop and deploy a fluorescent antibody test for detecting Legionella.
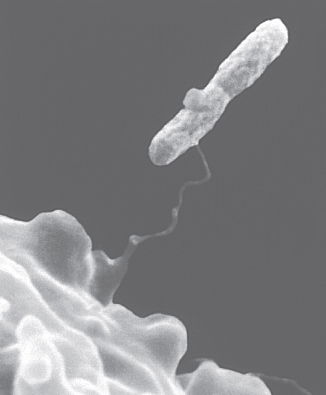
This electron micrograph depicts an amoeba, Hartmannella vermiformis (lower left) as it entraps a Legionella pneumophila bacterium (upper right) with an extended pseudopod
Legionella was now easily identified in situ, in vivo, and in vitro. Knowing the molecular and ecological basis of a pathogenesis helps one develop new ways to prevent and cure illnesses. For one thing, one can predict conditions under which pathogens are likely to thrive, spread, and cause illness. With improved techniques and molecular tools, fluorescent antibodies aid in diagnosis. A similar medical detective story is also true for the discovery and diagnosis of the agent causing Lyme disease. (See Body by Design, 2002, p. 145, for details.) Being a medical Sherlock Holmes helps one synthesize the diversity of facts into a unity.
Like Daniel in the Bible, one still seeks the Creator for guidance, direction, and solving enigmas. Detecting design in the world of biology is also like this. Design theory and order provide one with assumptions leading to the One who made us and the world around us. He can be a very present help in time of trouble, as in the day of Legionnaires’ disease. God can work through people like Dr. Fliermans to help solve practical problems. In the footsteps of Robert Koch, Fliermans successfully isolated a suspected pathogen from the wild and grew it in pure culture, proving beyond all doubt the specific element (Legionella) in an infectious disease (Legionnaires’). Like scientists of the Reformation era (e.g., Kepler), Dr. Fliermans sought to think after God’s thoughts (Ps. 139:17), being confident in God’s Word. His Word is true, and there is no final conflict between God’s world and God’s Word, as He is the author of both.
The Genesis of Germs
Professor Alan Gillen shows that constantly mutating diseases are proof for devolution rather than evolution.
Read Online
Answers in Genesis is an apologetics ministry, dedicated to helping Christians defend their faith and proclaim the good news of Jesus Christ.
- Customer Service 800.778.3390
- Available Monday–Friday | 9 AM–5 PM ET
- © 2026 Answers in Genesis

